 |
| Nursing Process |
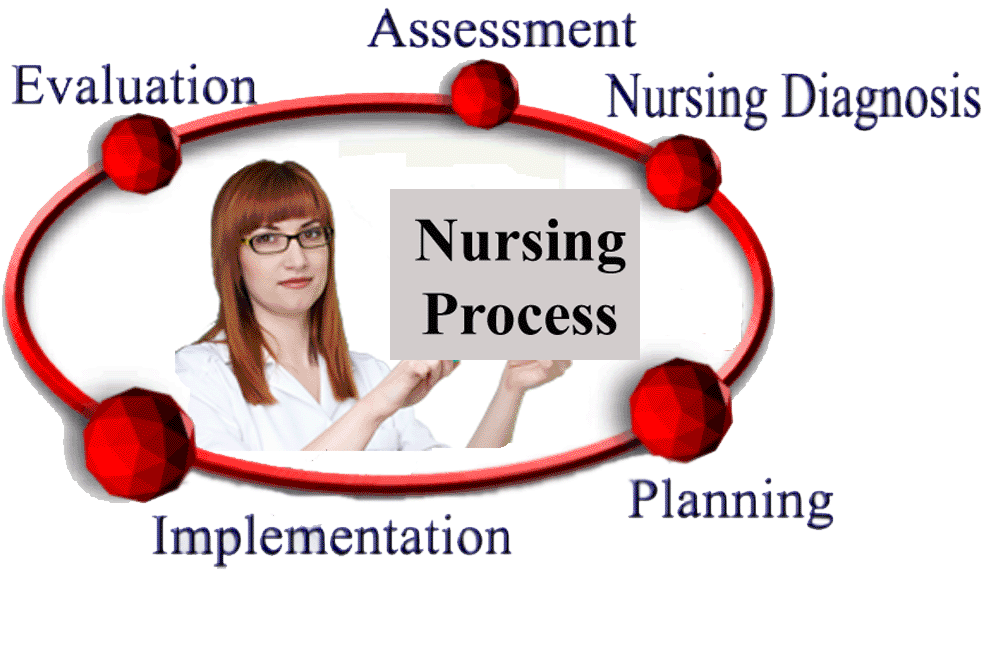
The nursing process is a problem solving process consists of elements assessment, planning, implementation, and evaluation. Many a priori assumptions have been identified and studied concern the nursing process approach to patient care that includes decision making as a characteristic of the process. These assumptions are that the nursing process is a holistic, scientific, individualized, problem-solving approach with an emphasis on diagnosing.
Shore (1988) described the nursing process as “combining the most desirable elements of the art of nursing with the most relevant elements of systems theory, using the scientific method.”
The nursing process is used by nurses every day to help patients improve their health and assist doctors in treating patients. Nursing requires the use of this process day in and day out. The process is based on theories and practices taught in nursing school. It is a form of problem solving. The nursing process is made up of a series of stages that are used to achieve the objective – the health improvement of the patient. The nursing process can stop at any stage as deemed necessary or can repeat as needed. This process is inclusive of physical health as well as the emotional aspects of patient health.
Nursing knowledge is used throughout the process to formulate changes in approach to the patient’s changing condition. During the process, nurses use this knowledge to identify problems and changes that are occurring to the patient. Caring for a patient requires the nurse to communicate with the patient to determine how they are feeling and gain the results of implemented care from the patient.
Phases of the nursing process include:
- Assessment of the patient’s needs
- Diagnosis of human response needs that nurses can deal with
- Planning of patient’s care
- Implementation of care
- Evaluation of the success of the implemented care
 |
| Nursing Process diagram Nursing Process diagram |
Nursing Assessment
Assessment is widely recognized as the first step in the nursing process. Nurses use assessment to determine patients actual and potential needs, the assistance patients require, and the desired outcomes to evaluate the care provided. Process includes using communication and physical assessment skills to establish a relationship and to gather needed information. The important content will vary with the patient but generally includes physical assessment, other diagnostic data, and assessment of the meaning of the health experience, quality of life, symptoms, and cultural factors that may affect health. Communication is essential in assessment, and is both the means for nurses and patients to influence each other and the process that leads to therapeutic and supportive influences on patients’ health. Patients’ successful communication of their needs to nurses is vital to individualized care. Individualized patient care has been found to produce more favorable outcomes and to reduce the cost of health care (Attree, 2001).
Physical assessment skills are routinely included in nursing curricula. They include (a) a general survey of patients’ appearance and behaviors; (b) assessment of vital signs, temperature, pulse, respiration rates, and blood pressure; (c) assessment of height and weight; and (d) physical examination to assess patients’ structures, organs, and body systems. Physical assessment can be complete, assessing all of the persons’ organs and body systems, or modified to focus only on areas suggested by the persons’ health history or symptoms. Effective assessment is the essential basis for providing effective nursing care.
Nursing Diagnosis
Nursing diagnosis is the second step in the nursing process. It is the judgment made about the meaning of a cluster of signs and symptoms (defining characteristics) found in the nursing assessment of the patient. Without a nursing diagnosis, a nurse is left rudderless to determine what goals should be set for the patient, what outcomes are desired, or what interventions to choose to meet the goals and resolve the nursing diagnosis.
NANDA, International (2003) defines a nursing diagnosis as a “clinical judgment about individual, family, or community responses to actual or potential health conditions/problems/life processes. A nursing diagnosis provides the basis for selection of nursing interventions to achieve outcomes for which the nurse is accountable”. There are three types of nursing diagnoses: actual, risk, and wellness.
An actual nursing diagnosis is a human response to health conditions/problems/life processes that exist in individuals, families, or communities. An actual nursing diagnosis is “supported by defining characteristics (manifestations, signs, symptoms) that cluster in patterns of related cues or inferences” (NANDA).
A risk nursing diagnosis describes a human response that may develop in vulnerable individuals, families, or communities. It is “supported by risk factors that contribute to increased vulnerability” (NANDA).
A wellness nursing diagnosis describes a human response that indicates a readiness for enhancement in levels of wellness in the individual, family, or community (NANDA).
The end product is the client diagnostic statement that combines the specific client need with the related factors or risk factors (etiology), and defining characteristics (or cues) as appropriate.
Planning
Planning includes setting priorities, establishing goals, identifying desired client outcomes, and determining specific nursing interventions. These actions are documented as the plan of care.
An intervention is defined as “any treatment, based upon clinical judgment and knowledge that a nurse performs to enhance patient/client outcomes” (Dochterman & Bulechek, 2004).
The Nursing Interventions Classification (NIC) is a comprehensive standardized classification of interventions that nurses perform. The Classification includes the interventions that nurses do on behalf of patients, both independent and collaborative interventions, both direct and indirect care. NIC can be used in all settings (from acute care intensive care units, to home care, to hospice care, to primary care) and all specialties (from critical care to ambulatory care and long-term care). NIC is recognized by the American Nurses Association (ANA).Nursing Outcomes Classification
The definition of a nursing-sensitive patient outcome is an individual, family or community state, behavior, or perception that is measured along a continuum in response to a nursing intervention(s). Each outcome has an associated group of indicators that are used to determine patient status in relation to the outcome. (Moorhead, Johnson, & Maas, 2004).
The Nursing Outcomes Classification (NOC) is a comprehensive, research-based standard ized classification of patient/client, family, and community outcomes developed to evaluate the effects of nursing interventions across the continuum of care. An outcome is stated as a variable concept representing an individual, family, or community condition that is measurable along a continuum and responsive to nursing interventions. The outcomes in the classification are grouped into seven domains: Functional Health, Physiologic Health, Psychosocial Health, Health Knowledge and Behavior, Perceived Health, Family Health, and Community Health. Within each domain are several classes that contain the outcomes specific to that class. The Nursing Outcomes Classification is the most comprehensive classification of nursing-sensitive patient outcomes currently available for nurses to use with individuals, families, and communities across the care continuum and in specialty practice.
Implementation
Implementation occurs when the plan of care is put into action, and the nurse performs the planned interventions. Legal and ethical concerns related to interventions also must be considered. Before implementing the interventions in Nursing care Plans, the nurse needs to understand the reason for doing each Nursing intervention, its expected effect, and any potential hazards that can occur. The nurse must also be sure that the interventions are
- Consistent with the established plan of care
- Implemented in a safe and appropriate manner,
- Evaluated for effectiveness, and
- Documented in a timely manner.
Evaluation
Evaluation is accomplished by determining the client’s progress toward attaining the identified outcomes and by monitoring the client’s response to/effectiveness of the selected nursing interventions for the purpose of altering the plan as indicated. This is done by direct observation of the client, interviewing the client/significant other, and/or reviewing the client’s health record.
Evaluation is an ongoing process, a constant measuring and monitoring of the client status to determine:- appropriateness of nursing actions
- the need to revise interventions
- development of new client needs
- the need for referral to other resources, and
- the need to rearrange priorities to meet changing demands of care.
To effectively use the nursing process, the nurse must possess, and be able to apply, certain skills. Particularly important is a thorough knowledge of science and theory, as applied not only in nursing but also in other related disciplines, such as medicine and psychology.




0 comments:
Post a Comment