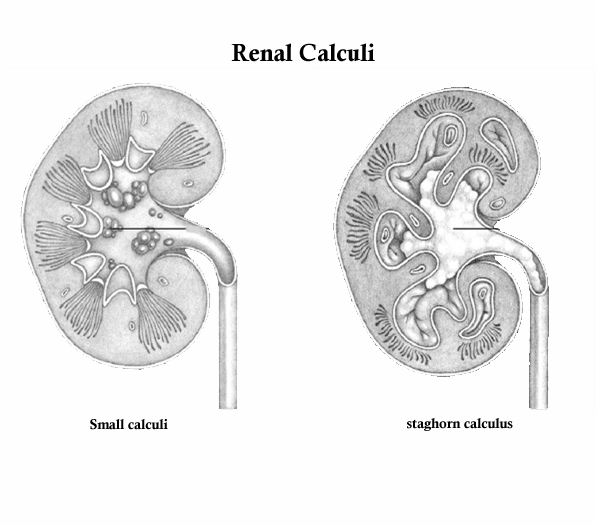
Renal Calculi/Kidney stones. Renal calculi, or nephrolithiasis, Kidney stones, are stones that form in the kidneys from the crystallization of minerals and other substances that normally dissolve in the urine. Renal calculi vary in size, with 90% less than 5 mm in diameter; some, however, grow large enough to prevent the natural passage of urine through the ureter. Renal calculi can form anywhere in the urinary tract, but they most commonly develop in the renal pelvis or calyces. Calculi may be solitary or multiple. Usualy these stones are composed of calcium salts. Other types are the struvite stones (which contain magnesium, ammonium, and phosphate), uric acid stones, and cystine stones. If the calculi remain in the renal pelvis or enter the ureter, they can damage renal parenchyma (functional tissue). Larger calculi can cause pressure necrosis. In certain locations, calculi cause obstruction, lead to hydronephrosis, and tend to recur. Renal calculi more common in males than females and are rare in blacks and children
Causes for Renal Calculi/Kidney Stones
The precise cause of renal calculi is unknown, although Renal Calculi/Kidney stones are associated with dehydration, urinary obstruction, calcium levels, and other factors.
- Metabolic conditions such as renal tubular acidosis, elevated serum uric acid levels Hyperparathyroidism, renal tubular acidosis, elevated uric acid, defective metabolism of oxalate, a genetically caused defect in metabolism of cystine, and excessive intake of vitamin D or dietary calcium may predispose a person to renal calculi.
- Urinary tract infections associated with alkaline urine have been linked with calculus formation. Cystine stones are associated with hereditary renal disease
- Dehydration. Decreased water excretion concentrates calculus-forming substances. Patients who are dehydrated have decreased urine, with heavy concentrations of calculus-forming substances. Urinary obstruction leads to urinary stasis, a condition that contributes to calculus formation.
- Infection. Infected, scarred tissue may be a site for calculus development. In addition, infected calculi (usually magnesium ammonium phosphate or staghorn calculi) may develop if bacteria serve as the nucleus in calculus formation. Struvite calculus formation commonly results from Proteus infections, which may lead to destruction of renal parenchyma.
- Changes in urine pH. Consistently acidic or alkaline urine may provide a favorable medium for calculus formation, especially for magnesium ammonium phosphate or calcium phosphate calculi.
- Obstruction. Urinary stasis allows calculus constituents to collect and adhere, forming calculi. Obstruction also encourages infection, which compounds the obstruction.
- Immobilization. Immobility from spinal cord injury or other disorders allows calcium to be released into the circulation and, eventually, to be filtered by the kidneys.
- Renal Calculi/Kidney stones occur more often in men than in women
Complications for Renal Calculi/Kidney stones
Calculi either remain in the renal pelvis and damage or destroy renal parenchyma, or they enter the ureter; large calculi in the kidneys cause pressure necrosis. Calculi in some sites cause obstruction, with resultant hydronephrosis, and tend to recur. Intractable pain and serious bleeding also can result from calculi and the damage they cause.
Possible Complications for Renal Calculi/Kidney stones:
- Decrease or loss of kidney function
- Scarring, Kidney damage,
- Obstruction of the ureter (acute unilateral obstructive uropathy)
- stones Recurrence
- Urinary tract infection (UTI)
- renal colic
Nursing Diagnosis for Renal Calculi/Kidney stones
Nursing Diagnosis nursing care plans for Renal Calculi/Kidney stones determine by what we found in nursing assessment.
Nursing Assessment nursing care plans for Renal Calculi/Kidney stones
Typically, assessment findings vary depends with the size, location, and cause of the calculi:
Patient history reveals a history of pain, and determine the intensity, duration, and location of the pain. The location of the pain varies according to the placement of the stone. The pain usually begins in the flank area but later may radiate into the lower abdomen and the groin. Ask if the pain had a sudden onset. Patients may relate a recent history of hematuria, nausea, vomiting, and anorexia. In cases in which a urinary tract infection is also present, the patient may report chills and fever. Determine the patient’s history to identify risk factors
Physical Examination.
Common symptom of renal calculi is severe pain, also referred as renal colic, which usually results from obstruction of large, rough calculi occlude the opening to the ureteropelvic junction and increase the frequency and force of peristaltic contractions. Pain intensity fluctuates and may be excruciating at its peak.
Patient with calculi in the renal pelvis and calyces may complain of more constant, dull pain. He may also report pain and severe abdominal pain. The patient with severe pain also typically complains of nausea, vomiting and, possibly, fever and chills. Hematuria occur when calculi abrade a ureter, abdominal distention and, rarely, anuria
Inspection reveals a patient in intense pain who is unable to maintain a comfortable position. Assess the patient for bladder distension. Monitor the patient for signs of an infection such as fever, chills, and increased white blood cell counts. Assess the urine for hematuria. Auscultate the patient’s abdomen for normal bowel sounds. Palpate the patient’s flank area for tenderness. Percussion of the abdominal area is normal, but percussion of the costovertebral angle elicits severe pain.
Psychosocial Assessment: Patients with renal calculi may be extremely anxious because of the sudden onset of severe pain of unknown origin. Assess the patient’s ability to cope. Since diet and lifestyle may contribute to the formation of calculi, the patient may face lifestyle changes. Assess the patient’s ability to handle such changes.
Diagnostic tests
Kidney-ureter-bladder (KUB) radiography, and
Excretory urography, retrograde pyelography,
Abdominal computed tomography scan, or
Abdominal or kidney magnetic resonance imaging
Kidney ultrasonography.
Urine culture of a midstream
Evaluated A 24-hour urine
Other diagnostic test:
Serial blood calcium and phosphorus levels indicate hyperparathyroidism and show an increased calcium level in proportion to normal serum protein levels.
Blood protein levels are used to determine the level of free calcium unbound to protein.
Increased blood uric acid levels may indicate gout.
Nursing diagnosis Nursing Care Plans for Renal Calculi/Kidney stones
Common nursing diagnosis found in Nursing Care Plans for Renal Calculi/Kidney stones
Acute pain
Altered urinary elimination
Deficient knowledge (treatment plan)
Impaired urinary elimination
Ineffective tissue perfusion: Renal
Risk for imbalanced fluid volume
Risk for infection Risk for injury
Sample Nursing Care Plans for Renal Calculi/Kidney stones
|
Nursing
diagnosis
|
Nursing
outcome
|
Nursing
Interventions
|
Evaluation
|
|
Acute pain related to
inflammation, obstruction, and abrasion of urinary tract by migration of
stones
|
·
Verbalizes
reduced pain level
|
·
Administer prescribed analgesic
·
Encourage
patient to assume position that brings some relief.
·
Reassess
pain frequently using pain scale.
·
Administer
antiemetic as indicated for nausea
·
Position the patient for comfort
|
|
|
Altered
urinary elimination
|
Urinary Elimination:
Ability of the urinary system to filter
wastes, conserve solutes, and
collect and discharge urine in a healthy
pattern
Urinary Continence: Control of the elimination of urine
Self-Care:
Toileting: Ability to toilet self
|
Assess degree of
interference/disability
·
Determine
client’s previous pattern of elimination and compare with current situation.
·
Frequency,
·
Urgency,
·
Burning,
·
Incontinence,
·
Nocturia/enuresis,
·
Size
and force of urinary stream.
·
Provides information about degree of interference with
elimination or may indicate bladder infection
· Palpate bladder to assess retention. Fullness
over bladder following voiding is indicative of inadequate emptying/retention
and requires intervention.
· Investigate pain which may be indicative of infection:
·
location,
·
duration,
·
intensity;
·
Presence
of bladder spasms, back or flank pain, etc.,.
· Determine client’s usual daily fluid intake
|
Verbalize understanding of condition.
● Identify causative factors. (Refer to
specific NDs for incontinence/retention as appropriate.)
● Achieve normal elimination pattern or
participate in measures to correct/compensate for
defects.
● Demonstrate behaviors/techniques to prevent
urinary infection.
● Manage care of urinary catheter, or stoma and
appliance following urinary diversion.
|




0 comments:
Post a Comment